Abnormal Blood Flow – Venous Reflux / Insufficiency
 When the one way valves fail or leak, gravity causes blood to flow backwards towards the feet and pool inside the veins. This backwards flow of blood is called “reflux”. Over time, the pooling blood causes excess pressure in the veins causing them to stretch and dilate. This dilation of the vein may cause pain, cause the legs to swell, ache, feel tired, heavy or full. Reflux of blood into the leg vein branches near the skin can also cause visible changes to the legs including spider veins, varicose veins, thickening and discoloration of the skin, and ulcers. Any impairment of blood flow back to the heart is referred to as venous reflux or venous insufficiency. Occasionally blockage of leg veins, due to blood clots or scarring, may alter normal blood flow.
When the one way valves fail or leak, gravity causes blood to flow backwards towards the feet and pool inside the veins. This backwards flow of blood is called “reflux”. Over time, the pooling blood causes excess pressure in the veins causing them to stretch and dilate. This dilation of the vein may cause pain, cause the legs to swell, ache, feel tired, heavy or full. Reflux of blood into the leg vein branches near the skin can also cause visible changes to the legs including spider veins, varicose veins, thickening and discoloration of the skin, and ulcers. Any impairment of blood flow back to the heart is referred to as venous reflux or venous insufficiency. Occasionally blockage of leg veins, due to blood clots or scarring, may alter normal blood flow.
Reflux of the superficial veins is the most common form of venous disease. In superficial venous insufficiency, the deep veins are usually normal. Blood from the deep veins may escape through refluxing perforator veins into the dilated superficial veins causing increased venous pressure in the superficial veins.
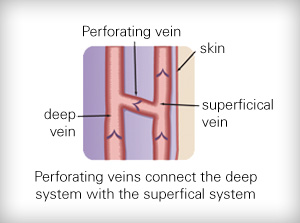 Changes in the legs due to venous reflux (varicose veins, spider veins, ulcers, pain, aching, etc) are typically caused by larger refluxing veins below the skin that may not be visible without specialized equipment. It is extremely important to evaluate all of the deep and superficial veins of the legs (not just the visible veins) to accurately identify all of the sources of reflux ensuring the most effective treatments to be prescribed.
Changes in the legs due to venous reflux (varicose veins, spider veins, ulcers, pain, aching, etc) are typically caused by larger refluxing veins below the skin that may not be visible without specialized equipment. It is extremely important to evaluate all of the deep and superficial veins of the legs (not just the visible veins) to accurately identify all of the sources of reflux ensuring the most effective treatments to be prescribed.
Causes of Venous Reflux
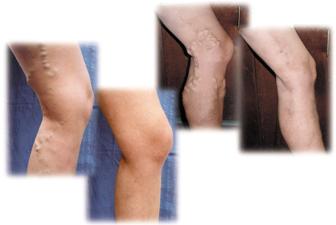 The cause of venous reflux is not yet fully understood. However, heredity plays an important part of this disorder. If one parent had venous disease, the chance of developing it is almost 50%. If both parents have venous disease, there is almost a 90% chance of developing the disorder or worsening the condition. Other factors that play a role in the development of venous reflux include:
The cause of venous reflux is not yet fully understood. However, heredity plays an important part of this disorder. If one parent had venous disease, the chance of developing it is almost 50%. If both parents have venous disease, there is almost a 90% chance of developing the disorder or worsening the condition. Other factors that play a role in the development of venous reflux include:
- Excessive body weight
- Prolonged standing or sitting
- Pregnancy, hormonal changes
- Advancing age
- Injury to the veins
- Blood clots
Signs and Symptoms of Venous Reflux
 Many patients experience symptoms of venous reflux such as:
Many patients experience symptoms of venous reflux such as:
- Leg pain, aching, tired or weak legs (especially after long periods of standing or sitting)
- Varicose veins
- Burning or itching of the skin
- Swollen legs and/or swollen ankles (edema)
- Restless legs and/or leg cramps
- Color and texture changes of the skin
- Open wounds (skin ulcers)
In the absence of symptoms, patients with cosmetic concerns due to the presence of varicose veins might be evaluated with only a physical examination. However, patients presenting with other symptoms of venous insufficiency should also undergo an in-depth evaluation, including a duplex ultrasound study.
Diagnosing Venous Reflux
 Venous duplex imaging uses ultrasound waves to create pictures. It allows visualization of the veins beneath the skin not visible to the naked eye. The Wisconsin Vein Center uses advanced state-of-the-art duplex ultrasound machines designed and developed by Terason. Duplex ultrasound provides visualization of a vein, which helps to identify if the vein is healthy or refluxing, if there are any blood clots in the vein, and provide an individual outline of the person’s venous system. By using ultrasound technology, underlying problems are diagnosed and a treatment plan is developed and tailored to a patient’s individual needs. This is an important part of achieving successful, long-term, therapeutic, and cosmetic results. The test is a non-invasive test and no preparation is needed. It takes approximately 30-60 minutes to complete and typically is a covered expense by most insurance companies.
Venous duplex imaging uses ultrasound waves to create pictures. It allows visualization of the veins beneath the skin not visible to the naked eye. The Wisconsin Vein Center uses advanced state-of-the-art duplex ultrasound machines designed and developed by Terason. Duplex ultrasound provides visualization of a vein, which helps to identify if the vein is healthy or refluxing, if there are any blood clots in the vein, and provide an individual outline of the person’s venous system. By using ultrasound technology, underlying problems are diagnosed and a treatment plan is developed and tailored to a patient’s individual needs. This is an important part of achieving successful, long-term, therapeutic, and cosmetic results. The test is a non-invasive test and no preparation is needed. It takes approximately 30-60 minutes to complete and typically is a covered expense by most insurance companies.
Duplex ultrasound is frequently used during different treatment methods. Advanced technology, specifically developed by Terason, allows the state-of-the-art equipment to be more compact allowing its use at the Wisconsin Vein Center.
Bleeding Vein – Hemorrhage
Significant hemorrhage or bleeding from a ruptured small varicose or spider vein in the lower leg in not uncommon. This usually occurs in longer standing venous insufficiency disorders when the blood pressure in the small veins in the lower leg increases significantly due to refluxing blood over a long period of time. It can also occur in older individuals as the skin becomes thinner and the subcutaneous tissue under the skin thins exposing the small veins to injury or dry skin conditions. Typically, these veins are dark, almost black and bulge a bit above the skin surface. These are usually located in the lower leg around the ankle surrounded by numerous other similar looking spider veins.
Bleeding can be profuse at times and is best managed emergently by putting your foot and leg as high as possible above one’s head(up against a wall or over the back of a couch), putting the tip of one’s finger on the bleeding site and applying pressure for about 15-20 minutes without peeking to see if bleeding has stopped. Once controlled, applying a small dime or nickel sized rolled up gauze/cotton ball plus a snug ACE bandage should control this situation until you can see your doctor or vein specialist. Such bleeding rarely happens in those wearing their medical grade compression stockings or after definitive treatment which may include injection sclerotherapy. Do not remain standing or in sitting position and try to control this bleeding. It will not work.
If you cannot control the bleeding with elevation and pinpoint pressure, you may need to summon help through your local hospital emergency room or by calling 911.
